Transforming Healthcare Finances
Medical Billing Services In Washington
If You're Seeing 30 Patients a Day and Still Struggling With Cash Flow.
Discover the easiest way to plug profit holes, slash admin burnout, and finally gain control of your cash flow. We don't sell services. Our Medical Billing Services In WA solve your billing pain.
Get a Custom Quote in 1 ClickRevenue Dashboard
+24.5%
$48,250
This Month
97.3%
Collection Rate
Claims Processed
1,248
Days in A/R
18 days

Increase Revenue
Up to 30% more

Save Time
20+ hours/week

Reduce Costs
Up to 50% less





 41% faster
41% faster
 15% increase
15% increase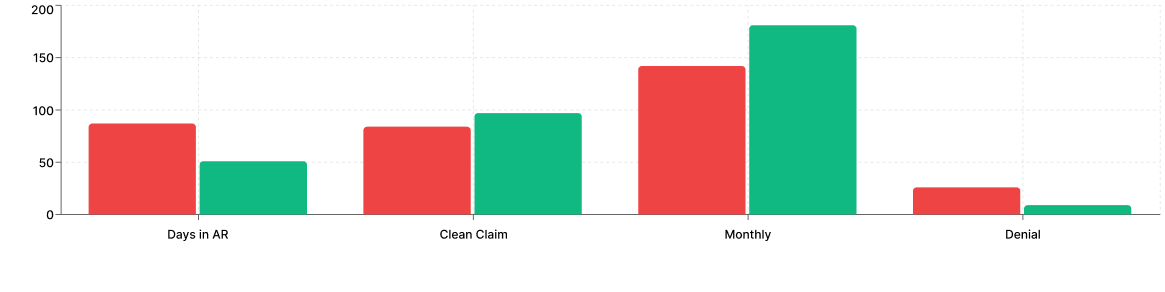
What Clients Say About Us
Below, you will find feedback from some of our cherished clients. We are proud to have helped them reach their business goals, and we appreciate the kind words they have shared about our services.
North Ocean Medical Group, P.C
5.0 Out of 5North Orchard Medicine PC
5.0 Out of 5Dr. Bryant Medical Practice PC
5.0 Out of 5Advanced Medical Office, PC
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5
5.0 Out of 5