Back pain has become a common societal problem. It affects millions of people around the world, leading to disability and missed days of work. For medical professionals, back pain is a challenge as it needs to be correctly diagnosed to ensure proper treatment. To help with this process, the International Classification of Diseases (ICD) has developed a code system for back pain ICD -10 code for back pain.
What is back pain?
It is a general term used to describe any discomfort or pain in the back, whether it is localized or widespread. Back pain can be caused by injuries, and degenerative conditions such as osteoarthritis, sciatica, disc herniation, and other disorders. In the USA, most back pain is due to muscle strain, ligament sprain, or joint problems.
Symptoms of Back Pain
Symptoms of back pain vary person to person. Generally, back pain can be described as aching or burning sensations, sharp pains that come and go, dull aches, tingling or numbness in the back area. Back pain can range from mild to severe, lasting anywhere from a few days to several weeks. Some of the common symptoms that trigger backpain are:
- Inactivity – back pain is more likely to occur when the back has not been used for a while
- Poor posture – poor posture can strain the back, leading to back pain
- Muscle tension or spasms – tightness in the back muscles can cause back pain and discomfort
- Obesity and excessive weight – extra weight can stress back muscles and lead to back pain
- Injury or trauma – back pain can be caused by injury or trauma, such as a fall or accident
- Osteoporosis – weakened bones can cause backache due to compression fractures in the spine's vertebrae.
Types of Back Pain
Back pain can be classified into two main types - acute back pain and chronic back pain. Some other important termonologies are also associated with back pain which are discussed below.
Acute Back Pain: Acute back pain is back pain that lasts less than three months. It can be caused by injury, muscle strain, bad posture, or other conditions.
Chronic Back Pain: Chronic back pain is back pain that has lasted more than three months. This type of back pain usually requires medical treatment and can indicate an underlying condition.
Different regions of back pain
The back is divided into three regions - upper back (thoracic), middle back (thoracolumbar) and lower back (lumbar). Each region can experience back pain differently.
Upper back pain is typically caused by poor posture, while middle back pain can be due to muscle strain. Lower back pain is usually due to back muscle strain, ligament sprains, herniated disks, or arthritis.
ICD 10 Code for Back Pain
M54.9 is reported as icd 10 code for back pain unspecified. This code is used to diagnose back pain, regardless of its cause or location. It may be accompanied by other codes when the back pain does have a specific cause such as an injury or trauma. In medical terminology, it is known as dorsalgia.
Low Back Pain Icd 10
Up until recently, the go-to ICD-10 code for back pain was M54.5 - a broad catch-all term that left room for interpretation and lacked specificity. But now, the Centers for Medicare and Medicaid Services (CMS) have taken action to improve patient care by discontinuing M54.5 and requiring providers to use more detailed, precise codes.
Why the change? Because one code cannot capture the complexity of every patient's back pain experience. By requiring more specific documentation, CMS is helping providers better understand their patient's needs and develop targeted treatment plans. So if you want to provide the best possible care for your patients with back pain, it's time to brush up on your ICD-10 coding skills and embrace the power of specificity.
Now, What To Code For Low Back Pain?
As healthcare providers, we know that keeping up with the latest codes and regulations can be a challenge. But when a code is eliminated, we need to be prepared with a replacement that meets the same level of specificity and detail. That's why the Centers for Medicare and Medicaid Services (CMS) has introduced a set of new, specified low back pain icd 10 codes to supplement the ones we already use.
- S39.012: This code describes a strain of the lower back's muscle, fascia, and tendon.
- M51.2-: This code describes a displaced disc in the thoracic or lumbar spine.
- M54.4-: This code describes a type of sciatica that affects the lower back and legs.
- M54.50: This code describes lower back pain that is not specified as related to the left or right side.
- M54.51: This code describes lower back pain that is specifically related to the left side.
- M54.59: This code describes lower back pain that is specifically related to the right side.
- S37.401A: This code describes an injury to the urethra and bladder following a traumatic event.
- S37.401D: This code describes a subsequent encounter for the same injury as S37.401A.
- S37.401S: This code describes a sequela (long-term effect) of the injury described by S37.401A.
ICD 10 Code for Upper Back Pain
In medical terms, CERVICALGIA refers to pain in the neck, shoulders, and upper back. Several conditions, such as poor posture, muscle strain, or herniated disks, can cause this. The ICD 10 code for this type of upper back pain is M54.02.
Tabular Representation of Back Pain ICD 10 codes
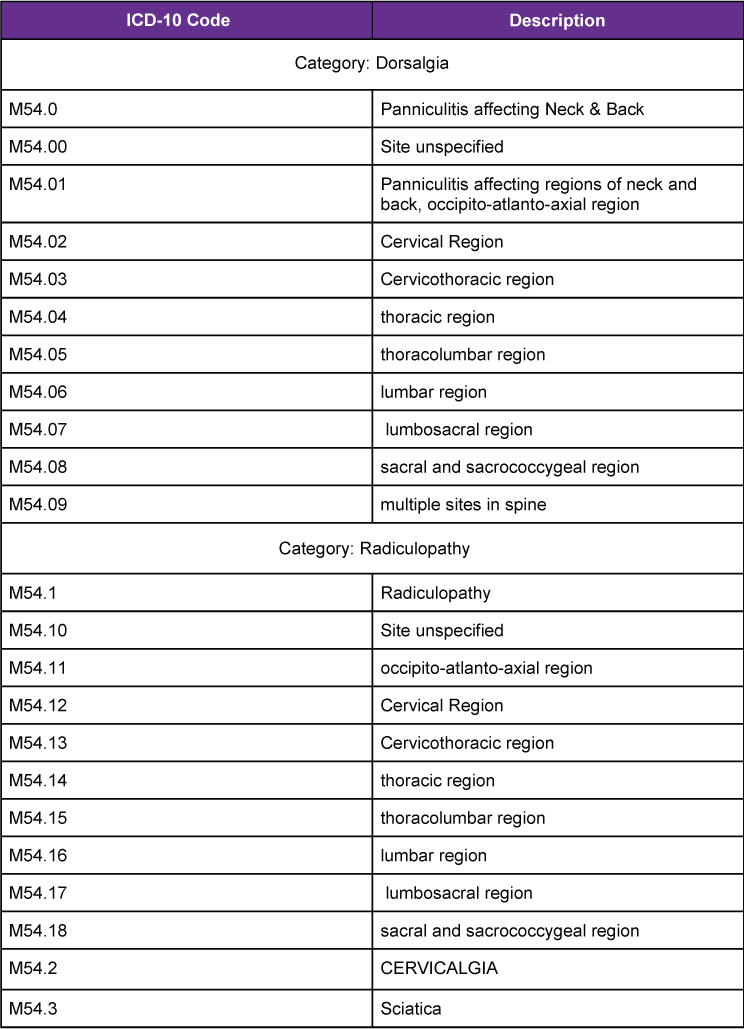
Final Words
Understanding the ICD-10 code for back pain is an important part of providing effective medical treatment. By familiarizing yourself with the codes above, you can ensure that your patient's diagnosis and treatment is accurately recorded in their medical records.
This will help you provide better care and specialized treatments when needed. Ultimately, this ensures your patients receive quality healthcare that meets their individual needs. By staying up-to-date with the latest codes and regulations, healthcare providers can ensure they are providing the best care possible for their patients.
With the new CMS guidelines in place, it's important to understand how the ICD-10 code for back pain is used in medical coding and billing. Stay in touch with HMS USA LLC to know more about ICD-10 coding updates and guidelines.
ABOUT AUTHOR

Grant Elliot
As a blog writer with years of experience in the healthcare industry, I have got what it takes to write well researched content that adds value for the audience. I am a curious individual by nature, driven by passion and I translate that into my writings. I aspire to be among the leading content writers in the world.