As a physical therapy healthcare provider, you know the importance of providing top-notch patient care. But did you know that maximizing your physical therapy billing units can significantly impact your bottom line?
In this insider's guide, you'll discover the secrets to unlocking the full potential of your billing units, allowing you to provide better care and boost your revenue. So, get ready to take your practice to the next level with the insider's guide to physical therapy billing units.
Contents
What are billing units in physical therapy?
Billing for Timed and Untimed Services
Billing for Individual Therapy vs Group Therapy
Example Case for Individual therapy
Example Case for Group Therapy
Billing for Overlapped or Multiple Appointments
Effective Tips to Follow for Billing Units for Physical Therapy Services
What are billing units in physical therapy?
Before diving deep inside as a healthcare provider, you must know how physical therapy services are billed. Physical therapy services are typically billed using a unit-based system, with each unit representing a specific amount of time spent providing treatment.
The number of units billed for a particular service is determined by factors such as the type of treatment, the session length, and the case's complexity. Standard physical therapy billing units include 15-minute increments and half-hour increments.
Billing units are used to standardize the billing process and ensure that healthcare providers are reimbursed fairly for the services they provide.
Billing for Timed and Untimed Services
Physical therapy services are usually categorized into two sets:
- Timed Services
- Untimed Services
Timed Services
Timed services are billed based on a set amount of time spent providing treatment, and 8 minute rule is applied to calculate billing units. Timed codes in physical therapy billing require the therapist to continuously attend to or maintain contact with the patient receiving the service. These services are typically highly interactive and hands-on, and as a result, they may offer higher reimbursement.
Some of the most common CPT Codes for Timed Services are:
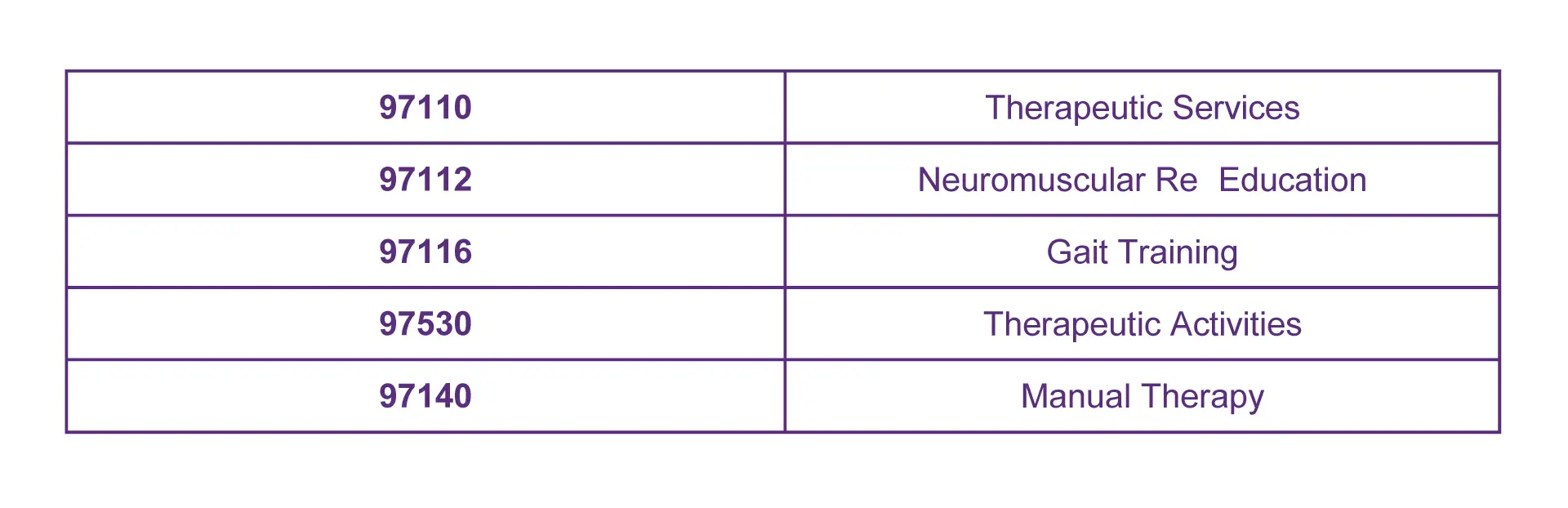

Untimed Services
As their name suggests, these services are not billed based on a set amount of time; instead, they are billed based on the complexity and type of service provided. For example, an evaluation or assessment service may be billed as a single untimed service, regardless of the time spent with the patient.
Some of the most common CPT Codes for Untimed Services are:
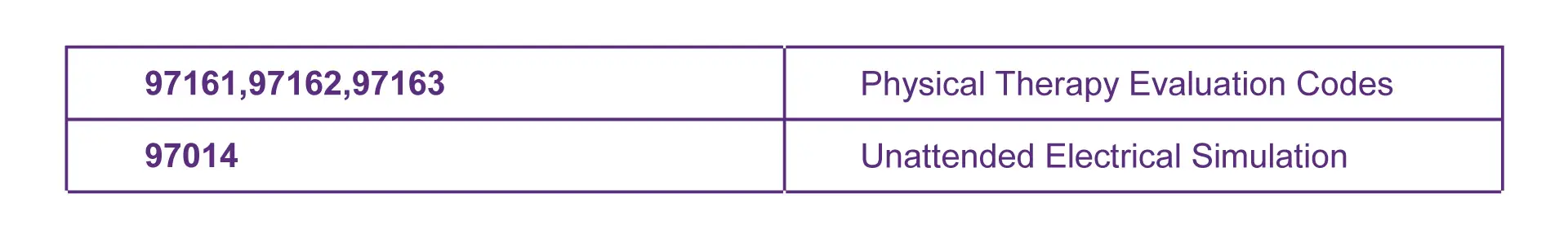

Physical therapy providers need to understand the difference between timed and untimed services to bill for them and ensure they are reimbursed fairly.
Billing for Individual Therapy vs Group Therapy
When providing direct one-on-one patient care, therapists bill for individual therapy and calculate the total minutes of service provided to each patient to determine the appropriate number of billing units for timed codes.
Direct one-on-one time may occur continuously or in distinct intervals. Each episode should be sufficient to effectively deliver the required skilled treatment based on the patient's care plan. Additionally, care delivery should differentiate it from treatment provided simultaneously to multiple patients.
Group therapy involves the same-time provision of services to two or more patients who may or may not be performing similar activities. When the therapist divides their attention among the patients, provides brief and occasional personal interaction, or delivers exact instructions to multiple patients simultaneously, it is appropriate to bill each patient who’s part of the group therapy with CPT 97150 (untimed service code)
It's important to note that group therapy's delivery should differ from individual therapy. In group therapy, the therapist may provide instructions and guidance to multiple patients simultaneously rather than giving each patient individualized attention.
This can be an effective treatment option for patients with similar conditions or goals, as it provides a supportive and interactive environment where they can work together toward rehabilitation.
Example Case for Individual therapy
Suppose 3 Patients, A, B, and C, enter the room and sit with the therapist. Patient A is given 8 minutes to discuss his current struggles and discuss how she feels. The therapist listens intently and offers tailored exercises for her to work on during the session. she agrees that she will practice these exercises independently while the therapist moves on Patient B for the next 8 minutes.
The therapist now turns to Patient B and provides the same attentive listening, analysis, and tailored exercises. After 8 minutes of constructive dialogue, the therapist moves on to Patient C for the remaining 8 minutes of one-on-one contact.
Once these initial 24 minutes are over, the therapist returns to Patient A to review the exercises and offer additional guidance. After 10 more minutes, she moves on to Patient B for 5 minutes and finally to patient C for 6 minutes. Throughout these periods of individual attention from the therapist, each patient is also provided time to practice their exercises independently.
After a successful therapy session, the therapist accurately bills each patient for the skilled time spent with them by assigning a 15-minute unit (based on 8 minute rule chart) of therapeutic exercise (97110).
Example Case for Group Therapy
During a 30-minute session, a physical therapist splits their attention between two patients, providing hands-on assistance for neuromuscular re-education to one and verbal cues for balance activities to the other. As the therapist is simultaneously treating both patients, this episode cannot be considered a one-on-one encounter, and each patient will be billed for one unit of group therapy (97150).
Billing for Overlapped or Multiple Appointments
Let's say two Medicare patients come in for physical therapy services, both seeking to improve their mobility and alleviate pain. The therapist, experienced in providing one-on-one care, has devised a well-rounded treatment plan for each patient, alternating between individual attention and supervised independent exercises.
At 10:00 a.m., the first patient, struggling with lower back pain, begins with a gentle warm-up routine. The therapist joins them to provide 15 minutes of manual therapy to loosen up their tight muscles. Meanwhile, the second patient, who is recovering from a knee injury, is provided with therapeutic exercises to improve their range of motion.
After 15 minutes, the therapist switches gears to give the second patient 10 minutes of one-on-one therapy, providing hands-on guidance for strengthening exercises. Meanwhile, the first patient continues to work independently, with the therapist periodically checking in to ensure they are performing the exercises correctly.
For the next 10 minutes, the therapist returns to the first patient to guide them through a series of targeted exercises, helping them to alleviate pain and increase their flexibility. Meanwhile, the second patient works under the therapist's supervision, performing self-stretching to maintain their progress.
Finally, the therapist spends 15 minutes with the second patient, providing hands-on guidance for therapeutic strengthening exercises. Both patients then conclude their treatment with 15 minutes of unattended electrical stimulation. After the session, both patients leave the clinic feeling empowered and confident in their progress.
In conclusion, the therapist will bill for two units of individual therapy for each patient and one separate unit for unattended electrical stimulation. It is important to note that the time spent by patients during self-stretching exercises is not considered billable.
Effective Tips to Follow for Billing Units for Physical Therapy Services
Maximizing your reimbursement for Physical Therapy services requires attention to detail and staying informed about the ever-evolving billing regulations. Here are some effective tips to follow for accurate billing of therapy services:
Familiarize yourself with Medicare billing guidelines
It is important to be knowledgeable about the regulations and guidelines set by Medicare for billing physical therapy services. This will help in ensuring that the billing is done correctly and efficiently.
Accurate record-keeping
Keeping a detailed record of the time spent with each patient is crucial for correct billing, and this will help ensure that the billing accurately reflects the services provided.
Avoid double booking and overlapping patients
To ensure that billing is accurate, it is important to avoid double booking or overlapping patients. This will prevent confusion and ensure that the time spent with each patient is accurately recorded.
Stay updated with billing code changes
Regular updates on billing codes and regulations are essential to keep up with the changes and ensure that the billing is done correctly.
Accurately reflect the care provided
It is important to ensure that the service being billed accurately reflects the care provided to each patient. This will help ensure that billing is done correctly and in compliance with the regulations set by Medicare.
Seek assistance from a billing specialist
If needed, consider seeking the assistance of a billing specialist. This will help ensure that the billing is done correctly and efficiently and can prevent potential mistakes or oversights.
Ending Words
So in last, we can say that having a proper understanding of physical therapy billing units is essential for healthcare providers to bill under any circumstances appropriately, whether it is for individual therapy or group; accurately billing those units and following the above-outlined tips will help providers to achieve max reimbursement and ultimately increase the practice bottom line.
Take your billing to the next level with the help of a professional medical billing company. HMS USA LLC offers top-notch services at an affordable rate, so don't let your practice fall behind. Join the ranks of successful healthcare providers and partner with us now!
ABOUT AUTHOR

Tammy Carol
As a blog writer with years of experience in the healthcare industry, I have got what it takes to write well researched content that adds value for the audience. I am a curious individual by nature, driven by passion and I translate that into my writings. I aspire to be among the leading content writers in the world.
