Most billing teams treat Place of Service codes like an afterthought. Pick a number. Move on. Submit the claim. That works fine until it does not. Then you are staring at a denial, a delayed payment, or a compliance audit that nobody saw coming.
POS 31 is one of those codes that looks straightforward on the surface but carries layers of nuance that can make or break a skilled nursing facility claim. Get it right and your reimbursements process cleanly. Get it wrong and you are chasing payments, filing appeals, and explaining errors to CMS.
This guide covers everything your billing team needs to know. No fluff. No filler.
What Is POS 31 in Medical Billing?
POS 31 stands for Skilled Nursing Facility in medical billing.
It is a two-digit Place of Service code entered on the CMS 1500 claim form to identify where a medical service was delivered. According to CMS, POS 31 is used when medical care is given in a Skilled Nursing Facility (SNF), a place where patients get professional nursing care, rehabilitation, or therapy after a hospital stay or for recovery from a serious health event.
Think of POS codes as the GPS signal on your claim. They tell the payer exactly where the service happened. The location changes everything from the payment rate to the coverage rules that apply.
POS 11 is a physician office. POS 21 is an inpatient hospital. POS 31 is a Skilled Nursing Facility. Each one triggers a different reimbursement calculation on the payer's end.
POS 31 Description: What CMS Actually Says
The official POS 31 description from CMS reads:
"A facility which primarily provides inpatient skilled nursing care and related services to patients who require medical, nursing, or rehabilitative services but does not provide the level of care or treatment available in a hospital."
Let that last part sink in.
A skilled nursing facility stay for Medicare beneficiaries is typically an inpatient rehabilitation stay following a qualifying inpatient hospital stay that was at least 3 days. The SNF fills the gap between acute hospital care and going home. Patients are still sick enough to need professional supervision. They just do not need the full resources of a hospital floor anymore.This is the setting POS 31 was built for.
Is POS 31 Inpatient or Outpatient?
This question comes up constantly. Let us settle it clearly.
POS 31 is considered an inpatient setting.
POS 31 is specifically indicated for inpatient medical services to a patient admitted to a skilled nursing facility. The patient is residing in the facility, receiving around the clock care under physician orders. That is inpatient by definition.
This matters because inpatient and outpatient settings carry different reimbursement rates. Billing POS 31 under an outpatient framework, or vice versa, will generate a mismatch that payers will catch and deny.
Is POS 31 a Facility or Non Facility?
Short answer: POS 31 is a facility setting.
Under Medicare's payment structure, facility and non facility rates differ significantly. When a service is rendered in a facility setting like an SNF, the practice expense component of the physician's payment is reduced. The assumption is that the facility itself absorbs overhead costs.
This directly affects how much your physician gets paid when billing under POS 31. Using a non facility rate in error can trigger overpayment recoupments during audits. It is not a small mistake.
What Qualifies as a Skilled Nursing Facility?
Not every nursing home qualifies for POS 31. This is a critical distinction that trips up even experienced billers.
A Skilled Nursing Facility (SNF) is a healthcare facility that provides medical care and rehabilitation services for patients who need more support than what can be offered at home but do not require full hospital care. These facilities are Medicare-certified, which means that they meet certain standards set by Medicare to ensure safe and high-quality care.
To bill under POS 31, the facility must be Medicare certified. If it is not, the claim will not hold up.
What Sets an SNF Apart from a Regular Nursing Home
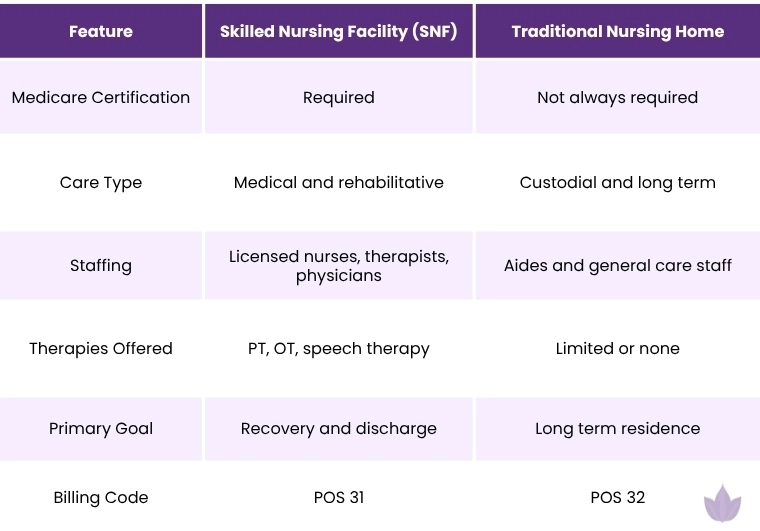
When to Use POS 31
POS 31 can be used in the following example scenarios: a physical therapist visits to provide rehab services after a major surgery to a patient shifted to an SNF, a physician visits a patient residing in an SNF for a follow up, or a psychiatrist visits to evaluate a patient admitted to an SNF for mental health stabilization.
Here is a more complete picture of when POS 31 applies:
Use POS 31 when all of the following are true:
✔ The patient is admitted to and residing in a Medicare certified SNF
. ✔ The patient is under an active Medicare Part A SNF stay.
✔ The service being billed requires a licensed medical professional (physician, therapist, nurse). ✔ Proper physician orders and clinical documentation support the visit.
Do not use POS 31 when:
✘ The care being provided is purely custodial (helping a patient bathe, dress, or eat).
✘ The patient's Part A SNF benefit has been exhausted.
✘ The facility is not Medicare certified. ✘ The patient has already transitioned to a long term stay beyond 100 days.
If the care is purely custodial, POS 31 should not be used. That would be POS 32.
POS 31 vs 32: The Comparison That Saves Claims
This is where most denials originate. Billers confuse POS 31 and POS 32 because the patient can be in the same physical building under both scenarios. The codes are not about the building. They are about the patient's coverage status at the exact moment of service.
The Clearest Way to Think About It
POS code 31 is used for all services furnished in SNFs for beneficiaries with Part A coverage. POS code 32 is used for all services furnished in nursing facilities, as well as services furnished in SNFs when beneficiaries have exhausted their Part A coverage.
|
Factor |
POS 31 |
POS 32 |
|
Setting |
Skilled Nursing Facility |
Nursing Facility |
|
Coverage |
Active Medicare Part A |
Part A exhausted or not applicable |
|
Stay Duration |
Typically up to 100 days |
Long term, post Part A |
|
Care Type |
Skilled medical and rehabilitative |
Custodial or maintenance care |
|
Reimbursement Rate |
Lower (facility rate) |
Higher (non facility rate) |
Yes, you read that correctly. POS 32 reimbursement is more than POS 31, so billers must be very careful when choosing to avoid fraudulent billing. This is exactly the pattern that draws CMS audits.
The 100 Day Rule
Skilled nursing facility stays can normally be a maximum of only 100 days. Typically if a patient starts a skilled stay (POS 31) and remains in the same facility after 100 days, the stay changes to a long term stay (POS 32).
One patient, one facility, two different POS codes over the course of their stay. This is real world billing complexity that requires active monitoring.
A Real Billing Trap to Avoid
Imagine a physician visiting a patient in a facility that houses both SNF and nursing facility residents. Same building. Same hallway. Two completely different billing rules depending on that specific patient's Medicare status that day.
It is imperative to confirm with the facility staff whether the patient is a skilled nursing patient or a nursing facility patient. There are not separate wings or areas designated as skilled or nursing.
If your biller does not verify before submitting, the wrong code goes on the claim. It is that simple and that costly.
Why POS 31 Codes Matter in Claims
Choosing the right POS code is not administrative paperwork. It is a financial and compliance decision.
Here is exactly why POS 31 accuracy matters to your revenue cycle:
1. It Determines Your Payment Rate
Payers use POS codes to calculate reimbursement. The wrong code changes the rate your practice receives. Sometimes you get underpaid. Sometimes you get overpaid, which triggers a recoupment later.
2. It Affects Compliance Exposure
Medicare has officially drawn the line: POS 31 or POS 32 must be on every physician claim for services in skilled nursing or nursing facilities or face denials and clawbacks. CMS has formalized enforcement through MM13767 (CR 13767), which took effect in July 2025. This is no longer a gray area.
3. It Triggers or Prevents Audits
After the Office of Inspector General discovered Medicare paid millions more for physician services at higher non-facility rates while enrollees were inpatients, CMS took steps to ensure proper POS code selection. Misusing POS codes puts your practice on the radar.
4. It Impacts Medical Necessity Documentation
Claims submitted with POS 31 require matching clinical documentation: physician orders, therapy notes, nursing records, and evidence of a qualifying hospital stay of at least three days. If the code and the documentation do not match, the claim falls apart.
This is why billing accuracy and proper medical coding services go hand in hand. One feeds the other.
Common POS 31 Billing Errors and How to Avoid Them
Even experienced teams make these mistakes. Knowing them in advance is your best defense.
Error 1: Using POS 31 After Part A is Exhausted
The moment a patient's Medicare Part A SNF benefit runs out, POS 31 no longer applies. Continuing to bill it after that point is incorrect billing. Switch to POS 32 and verify the patient's coverage status before every visit.
Error 2: Skipping the 3 Day Hospital Stay Requirement
Medicare requires a qualifying inpatient hospital stay of at least three days before Part A SNF coverage kicks in. If that stay did not happen, POS 31 claims for that patient will be denied.
Error 3: Using POS 31 for Custodial Services
Helping a patient with activities of daily living is not a skilled service. It does not qualify for POS 31. Only services requiring a licensed professional, like physical therapy, medication management, or physician evaluations, fall under this code.
Error 4: Vague Clinical Documentation
Notes should clearly describe what was done, how the patient responded, and the time spent. Entries like "patient seen" are too vague for insurers. Weak documentation is one of the fastest paths to a denial.
Error 5: Not Verifying the Facility's Medicare Certification
Always confirm that the SNF is actively Medicare certified before submitting a POS 31 claim. Certification can lapse. A lapsed facility means your claim has no foundation to stand on.
This is the kind of work that a qualified medical billing services team handles daily. The kind of operational alignment that protects your revenue before problems appear, not after.
How to Bill POS 31 Correctly: A Quick Reference Checklist
Before submitting any SNF claim under POS 31, confirm the following:
-
The facility is actively Medicare certified.
-
The patient had a qualifying inpatient hospital stay of at least 3 days prior to SNF admission.
-
The patient is under an active Medicare Part A SNF stay at the time of service.
-
The service being billed is a skilled clinical service, not custodial care.
-
Physician orders, therapy notes, or nursing records are complete and on file.
-
The stay is within the 100 day Part A benefit window.
-
The POS code on the CMS 1500 form matches the actual setting and patient status.
Missing even one of these items creates a vulnerability on the claim.
POS 31 and Its Impact on Revenue Cycle Management
POS 31 does not exist in isolation. It connects to nearly every other part of your revenue cycle.
It affects eligibility verification (you need to confirm Part A status). It ties to authorization workflows (some payers require prior auth for SNF services). It influences denial management patterns (SNF claims are among the most frequently audited). And it feeds directly into your reimbursement rates for the month.
This is why SNF billing is not a task to assign to the least experienced person on your team. It requires someone who understands the intersection of clinical documentation, payer rules, and CMS policy.
Practices that handle multiple nursing home accounts often find that partnering with a dedicated billing company dramatically reduces denial rates in this category. If your team is managing nursing home billing services at scale, having the right systems and expertise behind you matters.
And if you want to understand how assignment of benefits plays into these claims, our guide on AOB in medical billing covers the payment flow mechanics that connect billing accuracy to actual collections.
Final Thoughts
POS 31 is two digits on a form.
Those two digits determine whether your claim pays, denies, triggers an audit, or gets recouped months after you thought the account was closed.
The practices that stay out of trouble are the ones that treat POS coding as a clinical decision, not an administrative reflex. They verify. They document. They align their billing systems with real time facility data. And when the complexity of SNF billing outgrows what their internal team can handle cleanly, they bring in experts who live in this space every day.
If your SNF claims are generating more denials than they should, or if you want to make sure your POS 31 billing holds up under the tightened 2025 Medicare enforcement rules, our team at HMS USA LLC is here to help.
Talk to a billing specialist today and let us audit what your SNF claims are really doing.
ABOUT AUTHOR

Temba Altman
As a blog writer with years of experience in the healthcare industry, I have got what it takes to write well-researched content that adds value for the audience. I am a curious individual by nature, driven by passion and I translate that into my writings. I aspire to be among the leading content writers in the world.
