A patient walks in, receives care, and leaves. Three weeks later your billing team is staring at a denial. The coverage was inactive. The deductible had not been met. Nobody verified anything beforehand. That single oversight just cost your practice real money, and it happens thousands of times a day across the country.
This is exactly what VOB in medical billing is designed to prevent.This guide covers everything a healthcare provider, billing manager, or front desk coordinator needs to understand about the VOB process in medical billing, from the full form and definition to a step-by-step walkthrough, a real-world example, common challenges, and proven best practices for 2026.
What Is VOB in Medical Billing
The VOB full form in medical billing is Verification of Benefits. It is the process by which a healthcare provider, or their billing team, contacts a patient's insurance company before any medical service is rendered, to confirm that the patient is covered, what is covered, and what both the insurer and the patient are expected to pay.
Verification of Benefits (VOB) is the pre-service process of confirming a patient's active insurance coverage, plan-specific benefit details, financial responsibilities, and any prior authorization requirements before medical services are delivered.
In simpler terms, what is VOB in medical billing comes down to one core question: before you treat this patient, do you know exactly who is paying, how much, and under what conditions?
That answer shapes everything from claims submission accuracy to patient financial counseling. Without it, providers operate on assumptions, and assumptions cost money.
VOB vs. Eligibility Verification
Many providers use the terms interchangeably, but they are not the same. This distinction matters because misunderstanding it leads to incomplete pre-service checks and preventable denials.
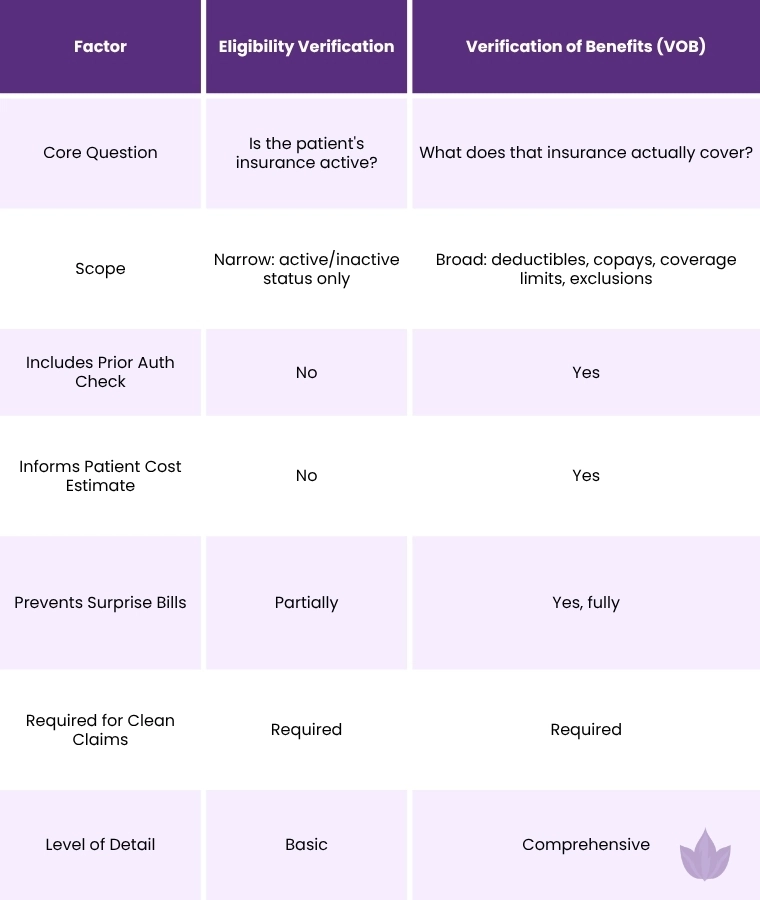
Think of eligibility verification as asking whether someone has a library card. VOB is asking what books they can borrow, how many at once, how long they can keep them, and whether any titles require special permission. Both questions matter. But only one gives you the full picture.
The Step-by-Step VOB Process in Medical Billing
The VOB process in medical billing follows a structured sequence that begins the moment a patient schedules an appointment. Here is how a complete, well-executed verification unfolds.
1- Collect Patient and Insurance Details
At the time of scheduling, gather the patient's full name, date of birth, insurance carrier, policy and group number, policyholder name if different, and any secondary insurance. Many practices collect this 48 to 72 hours before the appointment.
2- Contact the Insurance Payer
Reach out via the payer's provider portal, phone line, or Electronic Data Interchange (EDI) system. Each method has tradeoffs in speed and depth of information. Portals and EDI are generally faster; phone calls allow for nuanced clarification.
3- Confirm Policy Eligibility
Verify that the policy is active on the date of service. Confirm coverage effective dates, plan type, and whether the patient is listed as a covered member, not just the policyholder.
4- Review Benefit Details
Collect copay amounts, deductible status (how much has been met), coinsurance percentages, out-of-pocket maximums, covered services, and any exclusions relevant to the planned care.
5- Identify Prior Authorization Requirements
For procedures that require pre-approval, confirm whether a referral or authorization number is needed. Initiate the request immediately if so, to avoid service delays or post-claim denials.
6- Document and Communicate
Record all verified information in the patient's file and your EHR system. Share relevant details with billing staff, clinical teams, and the patient. Transparency at this stage prevents disputes later.
Industry best practice calls for initiating VOB 48 to 72 hours before a scheduled appointment. For high-cost procedures, surgeries, or mental health admissions, begin the process even earlier. For recurring patients on chronic care programs, re-verify at least once per plan year or whenever coverage information changes.
If your front desk team is stretched thin, HMS offers Virtual Front Desk services that include insurance verification support as part of a fully managed intake workflow.
A Real-World VOB in Medical Billing Example
Abstract concepts are easy to gloss over. Here is a concrete VOB in medical billing example that illustrates exactly what the process looks like in practice and what happens when it is skipped

Notice what that VOB accomplished. The practice knew exactly what to bill, the patient was not blindsided, prior auth was obtained before the scan, and the claim went out clean.
Now consider what would have happened without it: a claim submitted without the authorization number, a denial, weeks of appeals work, a frustrated patient, and lost revenue. That is the cost of skipping how to do VOB in medical billing correctly.
Why VOB Directly Impacts Your Revenue
The numbers tell a straightforward story.
For the average physician practice, that translates to thousands of dollars in revenue leakage every month. Here is what VOB insurance verification directly protects against.
1- Claim Denials: Inactive policies, lapsed coverage, missing authorizations, and uncovered services are all caught during VOB before they become denied claims.
2- Payment Delays: Clean claims get processed faster. VOB eliminates the back-and-forth of resubmissions and appeals that slow down your cash flow.
3- Write-offs and Bad Debt: When patient responsibility is established upfront, collections happen earlier and more reliably, reducing the volume of unpaid balances that age out.
4- Patient Surprise Bills: Patients who understand their financial obligation before a service are more likely to pay, and far less likely to dispute the bill or lodge complaints.
5- Compliance Risk: VOB ensures that prior authorization requirements are met, protecting the practice from payer audits and retrospective denials.
6- Coordination of Benefits Errors: For patients with multiple active policies, VOB identifies primary and secondary payers and establishes the correct billing sequence.
Denial management is a direct consequence of VOB failures. Read the HMS article on Home Health Denied Claims for a detailed look at what happens when pre-service verification falls through the cracks and how to recover revenue after a denial.
What Information Is Verified During a VOB Check
Not all VOB checks are created equal. A thorough verification covers a comprehensive set of data points, not just a quick eligibility ping. The following table outlines the key information collected during a complete VOB.
|
Category |
What to Verify |
Why It Matters |
|
Policy Status |
Active or inactive, effective and termination dates |
Billing an inactive policy guarantees a denial |
|
Deductible |
Annual deductible amount, amount met year-to-date |
Determines patient out-of-pocket before insurance pays |
|
Copay |
Per-visit or per-service copay amounts |
Needed to collect accurate payment at time of service |
|
Coinsurance |
Percentage split between payer and patient |
Affects patient cost estimate and billing accuracy |
|
Out-of-Pocket Maximum |
Annual OOP max and amount reached to date |
Once met, insurer covers 100%, patient owes nothing |
|
Service Coverage |
Whether the planned service is covered under the plan |
Prevents billing for non-covered services |
|
Network Status |
In-network vs. out-of-network for this provider |
Cost differences can be significant for the patient |
|
Prior Authorization |
Whether pre-approval is required; authorization number |
Missing auth is one of the top denial reasons |
|
Coverage Limits |
Visit limits, session caps, annual maximums |
Critical for mental health, rehab, and specialty services |
|
Coordination of Benefits |
Primary vs. secondary payer order for multi-policy patients |
Incorrect billing order triggers automatic denial |
Common VOB Challenges Healthcare Providers Face
Knowing what VOB is and knowing how to execute it perfectly in a real clinical environment are two different things. Practices across the country encounter the same recurring obstacles. Recognizing them is the first step toward building a process that overcomes them.
Long Hold Times with Insurance Representatives: Manual phone verification can mean 20 to 45 minute waits per call. Across a busy schedule, that quickly becomes an operational bottleneck that delays patient scheduling and strains administrative staff.
Inconsistent Information from Payer Representatives: The same policy can yield different answers depending on which representative you speak with. This is especially problematic for complex plans with carved-out benefits or tiered coverage structures.
Frequent Policy Changes: Patients change employers, switch plans, or have coverage gaps that are not reflected in real-time. A policy that was active during the last visit may have lapsed by the next one.
Data Entry Errors: A single transposed digit in a policy number or a misspelled name can cause a verification to fail or return incorrect information, which then carries forward into a claim denial.
Complex Coordination of Benefits: When patients carry two or more active policies, determining the correct billing order and understanding how secondary coverage responds requires expertise most front desk staff have not been formally trained in.
Rushed or Skipped Verifications: Under the pressure of high patient volume, VOB is the step most commonly abbreviated or deferred. The short-term time savings result in long-term revenue losses that far outweigh the original gain.
Outdated Insurance Information on File: Patients often forget to notify the practice when their coverage changes. Relying on information collected at a prior visit without re-verification creates compounding errors over time.
According to industry data, medical practices across the United States face denial rates of 12 to 15 percent annually due to incomplete or inaccurate eligibility and benefits verification. For a practice billing $2 million annually, that represents $240,000 to $300,000 in claims at risk each year, much of which may never be collected
How to Get VOB Right: The Case for Outsourcing
Knowing how to get VOB in medical billing right is one thing. Having the operational capacity to do it consistently, at scale, across dozens of payers and hundreds of patients per week, is another challenge entirely.
For many practices, especially solo providers and small- to mid-size groups, building and maintaining an in-house VOB infrastructure competes directly with clinical time and staffing budgets. The result is often a VOB process that works when things are quiet and breaks down under volume pressure.
Outsourcing benefit verification to a specialized billing partner solves several problems at once.
-
Access to dedicated verification specialists who perform VOB as a core function, not a side task, with training specific to complex payer requirements.
-
Faster turnaround times through established payer relationships, portal access, and automated verification technology that most individual practices cannot justify purchasing independently.
-
Consistent documentation standards across every patient encounter, ensuring audit-readiness and reducing the risk of claim disputes.
-
Scalability during high-volume periods without the overhead of additional administrative hires or the quality degradation that comes when existing staff are overloaded.
-
Reduced in-house operational costs by eliminating the training, rework, and revenue recovery work that an inadequate internal process generates.
At HMS USA LLC, benefit verification is handled as an integral part of a fully managed revenue cycle. From the moment a patient is scheduled, the verification workflow is active, thorough, and documented.
By the time the patient presents for their appointment, the practice already knows who is paying and what is covered. That is how to do VOB in medical billing at a standard that protects your revenue and your patients.
ABOUT AUTHOR

Temba Altman
As a blog writer with years of experience in the healthcare industry, I have got what it takes to write well-researched content that adds value for the audience. I am a curious individual by nature, driven by passion and I translate that into my writings. I aspire to be among the leading content writers in the world.
